Mast cells are one of the most ancient of immune cells. They’re foundational to the innate immune system, which is the first line of defense to any invading pathogen. However, they also help to orchestrate some of the behaviors of the newer adaptive immune system. What’s more, they are the sentinels of the body, stationed at every “crossroads” you can imagine, ready to release chemicals like histamines at the slightest provocation, whether that’s to help deal with a virus or in response to a physical injury.
Mast cells also communicate closely with the nervous system and are present both at the periphery and within the central nervous system (CNS). They are capable of inciting inflammation in reaction to signals from the nervous system and may be responsible for a number of idiopathic inflammatory diseases that can be psychosomatically driven.
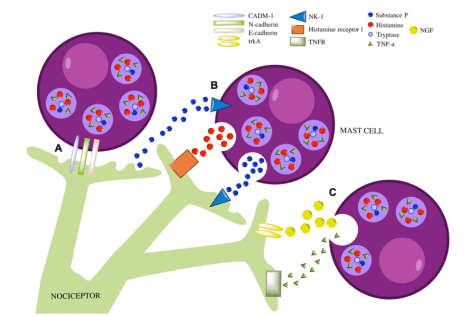
In addition to nerves, mast cells congregate around blood and lymphatic vessels where they communicate with and help regulate these systems as well. Mature mast cells are jacks of all trades, capable of phagocytosis (engulfing and eating other cells) and the production of modulators like cytokines, chemokines, and vasoactive substances.
But what happens when mast cells get too overstimulated? That can lead to inflammation and damage in whatever local tissue these mast cells reside in. But what happens when these mast cells are chronically overactive? This is called Mast Cell Activation Syndrome (MCAS). While the condition, Systemic Mastocytosis (SM), is the result of overproliferation of mast cells that then release too many mediators in the local tissue, MCAS, for now, is an idiopathic condition and is due to the mast cells being overactive. (Although sometimes modestly increased numbers of cells are noted in MCAS.)
Unfortunately, MCAS is such a new entity that doctors can’t yet agree on how to define it, which will continue to be worked out over the coming years. However, here’s some basics:
- Two or more organ systems are affected. These typically include (but aren’t limited to):
- the skin (flushing, severe itching, hives, swelling)
- the cardiovascular system (drop in blood pressure, sometimes leading to dizziness and even fainting)
- the respiratory system (asthma, coughing, wheezing, swelling of the throat)
- the gastrointestinal system (diarrhea, vomiting, bloating, cramping)
- the naso-ocular region (rhinitis, itching)
- anaphylaxis
- nervous system (anxiety, depression)
- One of more of the following blood or urine levels should be elevated during or around the time of symptom onset:
- tryptase
- histamine
- prostaglandin
- heparin
- chromogranin A
Interestingly, people with the connective tissue disorder, Ehlers-Danlos Syndrome Hypermobile Type, have frequent MCAS comorbidity, suggesting that mast cells may also target connective tissues leading to some of the symptoms of the condition [1]. Currently, some of our own work is addressing this possibility.
People with SM typically have an acute onset of symptoms, whereas people with MCAS usually have initial (though sometimes subtle) symptom presentation in childhood or the teenage years that progressively worsens into adulthood.
Often, people with MCAS have spells in reaction to stimuli, such as allergens, foods, medications, environmental chemicals (e.g., perfumes, cleaning products), temperature, and even emotional or physical stress.

The baseline treatment intervention for MCAS is a combination of high dose (2-4 x OTC) H1 and H2 antihistamines, but other medications are sometimes added, such as leukotriene receptor blockers and even psychoactive agents like tricyclic antidepressants or benzodiazepines, the latter both of which act on mast cells directly. Interestingly, many patients with MCAS react poorly to allergy shots, which are used in most allergists’ practices, so if you think you may have MCAS discuss treatment options with your physician cautiously and share this article that reviews laboratory assessment of MCAS.

Central nervous system vasodilation with histamine diphosphate, called “relief by flush,” was the treatment of choice for multiple sclerosis in this country in the 1950s (Current Therapy 1950-57, 1962). Between 1946 and 1959, more than 3000 patients with multiple sclerosis and other demyelinating diseases were treated with histamine diphosphate at the Multiple Sclerosis Clinic of St. Joseph Hospital in Tacoma, Washington. Most improved, some quite dramatically (Jonez 1952). Because the benefit of CNS vasodilation was never proved in controlled trials, its effectiveness has been largely forgotten. Yet histamine vasodilation consistently relieved acute attacks, and often the progression, of a disease now considered virtually incurable.
Jonez HD (with MZ Gross). My Fight to Conquer Multiple Sclerosis. NY: Julian Messner; 1952. (out of print but available through local libraries).
That’s very interesting, Peter. I wasn’t aware of that. Interesting also that histamines have a neuroexcitatory effect, acting through the NMDA receptor (and possibly other means).